At The Ear Nose Throat-Head & Neck Centre, we are able to diagnose, manage and treat the following conditions:
- Superficial and total parotidectomy for parotid tumours with facial nerve preservation
- Excision of submandibular gland for tumours and stones
What are some of the reasons for Parotid surgery?
The parotid glands are a pair of major salivary glands located in front of the ear and slightly below it. Parotid surgery, or parotidectomy, is a surgical operation to remove part of or the whole parotid gland. Most patients who require this operation will have the following conditions: growth or tumour, chronic infection (known as sialdenitis), or obstruction of the saliva flow due to stones.
Most salivary gland tumours occur in the parotid glands (the other salivary glands being the submandibular and sublingual glands). Of the parotid gland masses, 75% are tumours, of which 80% are benign (non cancerous). The most common benign parotid tumour is a pleomorphic adenoma. Benign parotid tumours are generally more common in women than men, except for Warthin’s tumour which is usually found in older male smokers. Most patients with benign tumours present with a painless slow growing swelling of the cheek area. This may be bilateral and even go unnoticed for a long time.
Photo of patient with a large parotid tumour
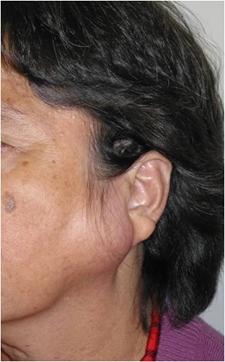
What are the procedures for Parotidectomy (Parotid surgery)?
A full history and clinical examination will be required. Palpation of the gland and the duct will be performed, as well as the presence of any enlarged lymph nodes in the neck. Baseline facial nerve function will be tested clinically.
Ultrasonography is a useful diagnostic investigation especially when combined with Fine Needle Aspiration or Core Needle biopsy. High-resolution CT scans is the investigation of choice if stones are suspected but not palpable on clinical examination. If a salivary gland tumour is present, CT and/or MRI scans may be necessary to assess the extent of the tumour and possible involvement of the surrounding structures.
While most of the parotid tumours are benign, patients may often still require parotid surgery. This is because lumps such as pleomorphic adenoma will continue to grow and have potential for malignant change i.e. it can become cancer after many years (usually as a carcinoma ex-pleomorphic). Some patients also find that the lump is very unsightly.
Parotidectomy is performed under general anesthesia. After the surgery, a drain will be sited to prevent any accumulation of blood within the tissues. It usually takes about 2-3 days before the drain is removed. Most patients will be required to stay in hospital for only 1-3 days postoperatively.
While parotid surgery is generally considered a safe procedure in trained and skilled hands, there are still possible complications and risks, as with all other surgeries. The most common are post-operative bleeding, injury to the facial nerve causing facial weakness (facial asymmetry e.g. drooping of the corner of the mouth causing a wry smile), facial indentation (one side of the cheek is flatter than the opposite side), temporary numbness of the face and ear, or Frey’s Syndrome (food-induced flushing and sweating on the skin of the cheek just in front of the ear).
The risks and benefits have to be weighed prior to any surgery, but generally the risks connected with the surgery are considered minimal compared to not having the tumour removed. In addition, most of the complications are transient and will only last for several days to weeks. You should discuss any concerns you have with the doctor any at point in time.
What are salivary gland stones?
Similar to how some individuals are predisposed to gallstones and urinary tract stones, stones can also arise in the salivary glands or their respective ducts. 90% of salivary gland stones arise in the submandibular gland, usually within the duct. Others involve the parotid gland itself, or the minor salivary glands.
What are the causes and symptoms of salivary gland stones?
Dehydration, medications, and trauma are thought to be risk factors in the formation of stones. These salivary gland stones are composed chiefly of calcium salts.
Patients typically presents with pain and/or swelling. These symptoms may be intermittent and be exacerbated by meals or the thought of food. If pus is seen from the duct opening, with redness of the skin over the gland, fever and chills, this may suggest acute sialadenitis or acute infection of the salivary gland.
What are the treatment options for salivary gland stones?
A full history and clinical examination will be required. Palpation of the gland and the duct will be performed to identify any stones or abnormal masses.
High-resolution noncontrast CT scan is the investigation of choice if stones are suspected but not palpable on clinical examination. Ultrasonography is a useful alternative investigation.
Other conditions to consider include infection, tumors, Sjögren’s syndrome, sarcoidosis, malnutrition and chronic alcoholism.
Conservative management for stones includes over the counter pain medications, adequate hydration, applying heat and massage, “milking” the duct, and sucking on sour candies to promote salivary flow. Surgery is usually reserved for patients with recurrent stones or failed minimally invasive procedures. There is a very small risk of injury to the lingual, hypoglossal, and facial nerves.
Acute sialadenitis require antibiotic treatment and resolve within 7-10 days. Failure to resolve may suggest an abscess which can be identified on CT scan and usually require a drainage procedure. Severe cases may lead to airway compromise and difficulty breathing.
Please contact us if you have further enquiry on Parotid and Salivary Gland Lumps or Request an appointment to see our ENT specialist
